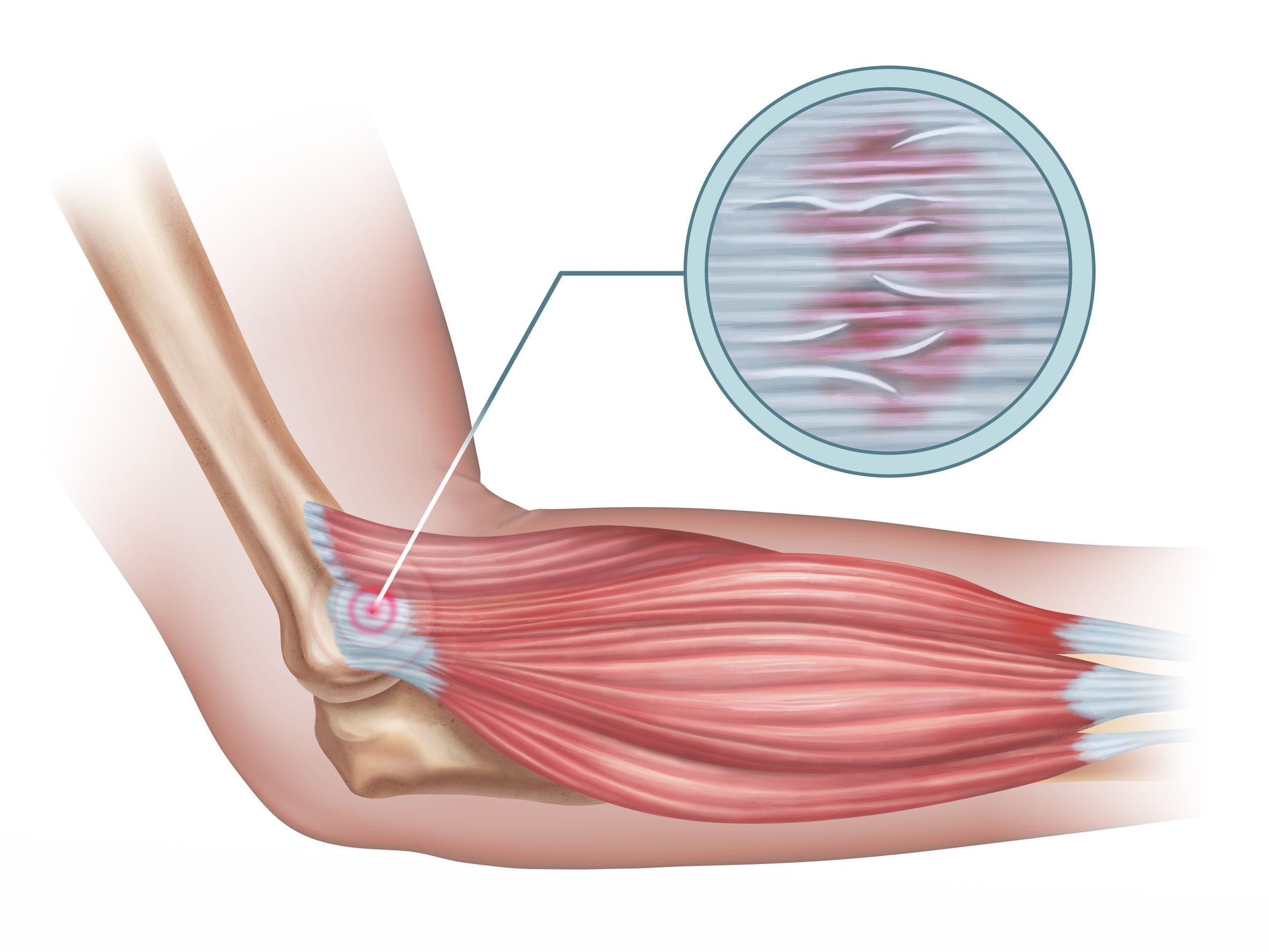
Tendinitis vs. Tendinosis: What’s the Difference? And 8 Steps to Recovery
Injuries to tendons are not only painful, but they can be very frustrating for two reasons. One, they are slow to heal and two, a change in behavior is often required in order to allow the healing process to take place. Many tendinopathies (which include tendinitis, tendinosis, and tenosynovitis) result from repetitive use, and whether the activity that caused the tendinopathy is work-related or recreational, it is usually difficult to avoid.
In this post we’ll discuss the difference between tendinitis and tendinosis, and the most effective 8-step approach to recovery.
What is a tendon?
Tendons are a type of connective tissue that serve the important function of connecting muscles to bones. They’re made up of densely packed collagen fibers arranged in parallel along with a small amount of a protein called elastin, which allows tendons to return to their normal length after contracting or stretching.
In comparison to muscles, tendons are relatively poorly vascularized, meaning they have less blood flow. This means that injuries to tendons take longer to heal than injuries to muscles, and is a reason why tendon injuries are so frustrating. Research suggests that it can take anywhere from 6 weeks to 9 months for tendon injuries to fully heal.
The important difference between tendinitis and tendinosis
Tendon pain resulting from repetitive use has long been diagnosed as tendinitis, but research increasingly shows that these cases are most often actually tendinosis.
Tendinitis, as designated by the suffix “itis,” is an acute, inflammatory condition. True tendinitis usually occurs when a tendon is overloaded by a sudden or heavy force, resulting in micro-tears in the tendon. The immune system kicks in to repair the damaged tissue, and the tendon and surrounding tissues become swollen and painful.
Tendinosis, as designated by the suffix “osis,” is a chronic, degenerative condition. In tendinosis, the tendon’s collagen degenerates in response to chronic overuse. Even small movements, like clicking a computer mouse or texting, can result in tendinosis over time. In tendinosis, inflammation is not present, and the shiny, firm, white tendon has become dull, soft, and brown.
Researchers have learned about this important difference between tendinitis and tendinosis by examining surgical patients who are diagnosed with tendinitis. For example, in a study of people diagnosed with tennis elbow, no signs of inflammation were found, and thus the correct diagnosis for these patients was tendinosis.
Tendinitis is painful because inflammatory substances activate nociceptors (pain receptors), and because the swelling present in inflammation can cause painful pressure. But if inflammatory substances aren’t present in tendinosis, why is it painful? Research shows that degenerating tendons contain high levels of the amino acid glutamate, and it’s likely that this is at least partly responsible for the pain.
Another study examined patients with painful Achilles tendinosis and found neovascularization present in all of the painful tendinosis tendons, but in none of the pain-free controls. This finding suggests that the growth of new blood vessels in degenerative tendons plays a role in the pain felt in tendinosis.
If your tendon pain has come on gradually, and if it seems to be the result of repetitive use, it is most likely tendinosis. In the next section we’ll discuss a multifaceted approach to healing tendinosis based on proven methods.
The most effective 8-step approach to healing your tendinosis
Tendinosis is a frustrating condition to deal with because it can take a long time to fully heal, and behavior and lifestyle modifications are often required in order to allow it to heal. So while you may be resistant to doing everything recommended below because it seems like too much work, keep in mind that degenerative tendons are at increased risk for rupture—and that’s something that you definitely want to avoid.
Take the time and effort to let your painful tendon heal, and you’ll likely learn some valuable things about how to take care of yourself and prevent future tendon problems from developing.
Note that anti-inflammatory medications are generally not recommended for tendinosis, as inflammation is not present.
1. Reduce or avoid the repetitive activity that caused the tendinosis. If the activity is required at your job, make sure to take frequent breaks, like a 5-minute break every 20-30 minutes. If possible, train yourself to do the task by using your body in a different way—like with your non-dominant hand—so that the injured tendon can rest.
If the activity is recreational, I recommend stopping it altogether until your pain subsides. If you’re an athlete, do a different type of exercise that doesn’t aggravate your painful tendon, and even better, use this as an opportunity to create a cross-training regimen for yourself. I recommend alternating at least 3 different types of workouts throughout the week that use your body in different ways; this is the best way to avoid overuse injuries while maintaining a high level of physical fitness.
2. Adjust ergonomics and biomechanics. If the repetitive activity that caused your tendinosis is performed at your job, then take the time to evaluate how your workstation is set up. Sometimes a small change, like moving your keyboard so that your wrists are in a neutral position when typing, can have a huge impact.
Whether your tendinosis was caused by a work-related or recreational activity, consider how you might be able to use your body differently in order to avoid straining the painful tendon. Tendinosis can occur not just from overuse but also from misuse—moving in an unnatural or imbalanced way, or with too much force. Clinical Somatics exercises are extremely effective for retraining habitual posture and movement. They also give you fine-tuned control of your body so that you can sense when your posture or movement is the slightest bit “off” and correct it before pain or damage occurs.
3. Support and splint the painful tendon. Limiting movement by taping or wearing a brace reduces the amount of harmful, repetitive movement that caused the injury. If you must continue to do the repetitive task at work, supportive tape or a brace is recommended.
4. Apply ice. Icing degenerative tendons is not intended to decrease inflammation, as there is none in tendinosis. Instead, ice is recommended for painful tendinosis because it has proved beneficial in clinical settings. The reasons why are not fully understood, but it may be because ice constricts blood vessels. Abnormal vascularization (growth of new blood vessels) is common in tendinosis, and as mentioned earlier, may contribute to the pain.
5. Massage the painful area. Massage has many benefits for healing connective tissue because:
- It stimulates circulation
- It stimulates fibroblast activity, speeding up the generation of new collagen
- It reduces scar tissue formation
- It temporarily relaxes the attached muscle, reducing strain on the tendon
- It temporarily decreases pain sensation
6. Get proper nutrition. Since the key to healing a degenerative tendon is allowing sufficient collagen to be produced—and not subsequently worn away by repetitive movement—it’s important to get enough of the vitamins and minerals that play a role in collagen synthesis and tissue repair. While more research is needed, a quick internet search will give you the basics: A diet rich in vegetables, fruits, legumes, nuts, seeds, and whole grains will provide you with the nutrients and antioxidants needed for optimal healing.
An important note: The collagen found in popular supplements is broken down into amino acids in our digestive system, and then our body uses the amino acids wherever they’re needed. So as long as you’re getting protein from varied sources in your diet, collagen supplements are probably a waste of money.
7. Release your muscles. Tight muscles pull on their tendons, creating excess strain on the tendons. This strain contributes to tendon degeneration and increases the risk of tendon rupture. An important part of both the healing and prevention process is reducing the baseline level of tension in your muscles.
While you might be inclined to focus on releasing just the muscle that’s attached to your painful tendon, keep in mind that one single muscle is never responsible for a dysfunctional movement pattern. You should reduce muscle tension throughout your body so that you can improve your posture and movement and prevent recurring and new problems. Don’t waste your time with static stretching—pandiculation is the most effective way to reduce your muscle tension.
8. Practice eccentric strengthening. An eccentric contraction is the action of a muscle lengthening while still contracting under load; an example is your biceps muscle slowly elongating as you lower a dumbbell. A number of studies have shown the effectiveness of eccentric strengthening as a treatment for tendinosis, and there are several likely reasons why. First, scientists believe that eccentric strengthening stimulates collagen production in tendons. Second, animal experiments have shown that eccentric strengthening can improve collagen alignment and stimulate collagen cross-linkage formation, improving the tensile strength of the tendon.
Lastly, scientists recognize that eccentric contraction actually lengthens muscle, thereby reducing muscle tension and strain on the attached tendon. Pandiculation is a specific type of eccentric contraction, the sole purpose of which is to reduce muscle tension rather than build strength. Yet another reason to incorporate Clinical Somatics into your regimen for tendinosis recovery!
Recommended reading:
The Pain Relief Secret: How to Retrain Your Nervous System, Heal Your Body, and Overcome Chronic Pain by Sarah Warren, CSE
Somatics: Reawakening the Mind’s Control of Movement, Flexibility and Health by Thomas Hanna