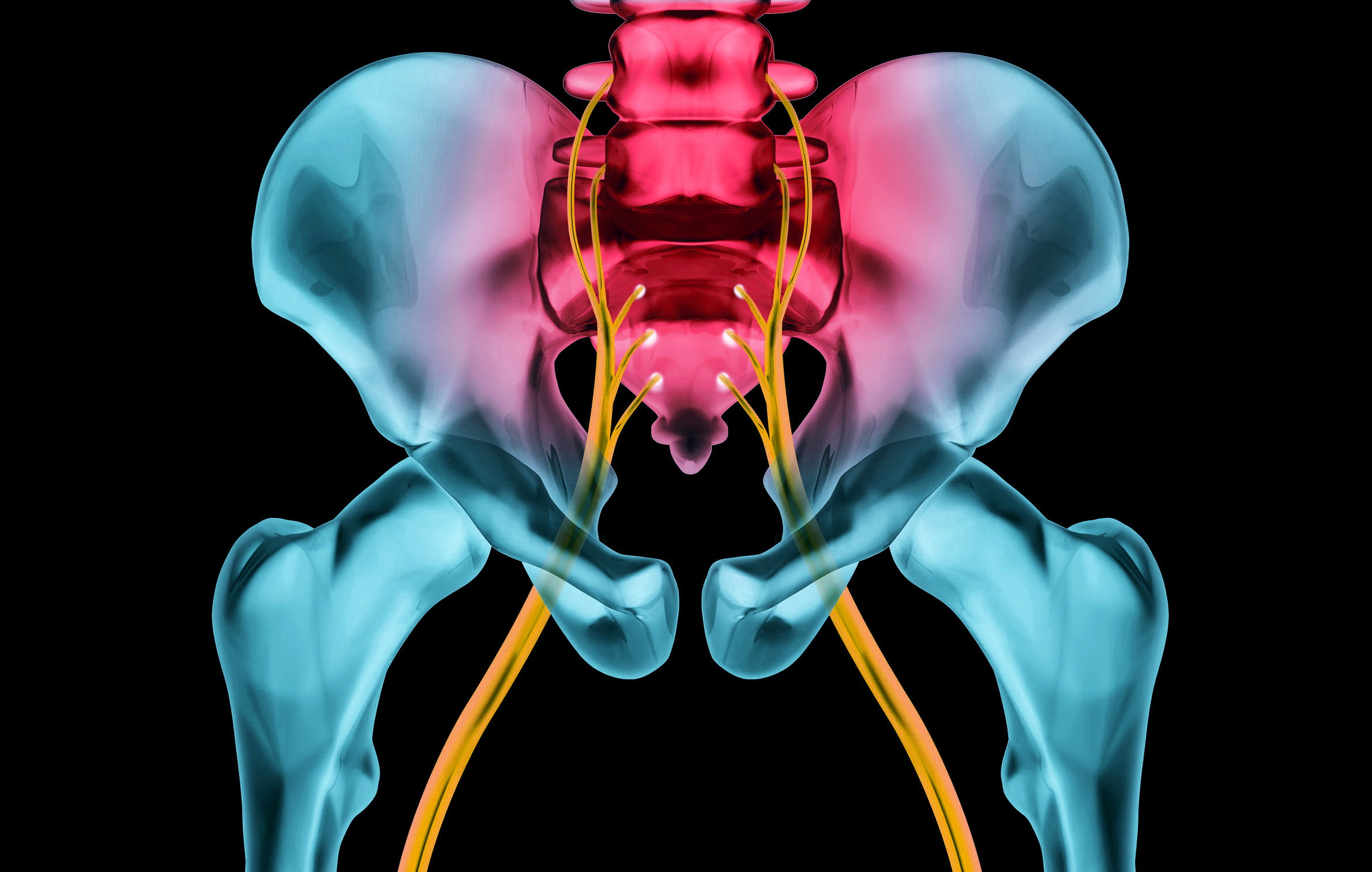
The Functional Cause of Sciatica
Sciatica often occurs along with back pain, which 80% of Americans will experience at some point in their lives. By the time your doctor diagnoses you with sciatica, the cause may appear to be structural—most commonly, a herniated disc pressing on the root of the sciatic nerve.
However, as you’ll learn in this post, this structural issue begins with your function: how you’re sitting, standing, and moving every day, and the patterns of muscular tension that you develop as a result. Many cases of sciatica can be eliminated, and virtually all can be prevented, by releasing the chronic muscle tension in the lower back that compresses the lumbar discs and the sciatic nerve.
What is sciatica?
The sciatic nerve is the largest and thickest nerve in the human body. Nerves exiting the spine between the fourth lumbar vertebra and the third sacral vertebra come together to form the sciatic nerve, which runs through the buttocks and all the way down each leg. The sciatic nerve is responsible for much of the sensation and motor control of the legs and feet.
Sciatica symptoms are generally caused when the nerves exiting the spine are compressed between the vertebrae by a bulging or herniated disc pressing against the nerve roots. Symptoms can also occur if the sciatic nerve is compressed after it has exited the spine. When your sciatic nerve is compressed you may experience the following symptoms:
- Pain radiating from the lower back into the hip and down the leg
- Shooting pain or a burning sensation in the leg and foot
- Pain that becomes worse when sitting
- Tingling, numbness, or weakness in the leg and foot
- Difficulty moving the leg
In a small portion of the population, the sciatic nerve runs through a gluteal muscle called the piriformis instead of underneath it. For these people, chronic tightness in the piriformis can compress the sciatic nerve, causing piriformis syndrome. The symptoms of sciatica and piriformis syndrome are generally the same; the distinction is made based on where the nerve compression occurs.
What causes sciatica?
In about 90% of cases, sciatica is caused by a herniated disc compressing the root of the sciatic nerve. Other causes include degenerative disc disease, spinal stenosis, spondylolisthesis, pregnancy, tumors, or infection.
However, sciatica almost always begins as a functional issue. When tight lower back muscles constantly compress the lumbar spine, or when the lumbar spine is compressed repetitively by heavy lifting or poor body mechanics, structural changes begin to occur. Lumbar discs thin and herniate, vertebrae move out of alignment, the spinal canal may narrow, and bone spurs can develop.
These painful, sometimes permanent structural issues most often occur simply because of the way we use our bodies.
Some warning signs to be aware of are:
- Lower back tightness or pain
- Mild tingling or occasional numbness in the leg, foot, or toes
- Imbalanced body mechanics or posture, such as functional uneven leg length or scoliosis
Why do we develop the chronic muscle tension that compresses the lumbar spine?
The lower back muscles are core muscles: the strong muscles at the center of our body that initiate and control our movement and posture.
Full-body movements begin with movement of our pelvis, carried out by our lower back and abdominal muscles. These core muscles provide essential control and stability as we move. Our standing and sitting posture also develops based on how we hold our pelvis when we’re not moving.
Since we’re always using our lower back muscles, and often demand that they perform repetitive or powerful actions, it’s very common for them to become chronically tight. Here’s why:
The movement and level of contraction of our muscles is controlled by our nervous system. The way that our muscles move, and how much we keep them contracted, is actually learned over time by our nervous system.
Our nervous system learns certain ways of using our muscles based on how we choose to stand and move each and every day. Our nervous system notices the postures and movements that we tend to repeat, and it gradually makes these postures and movements automatic so that we don’t have to consciously think about them. Part of this process of automation is that our nervous system starts keeping certain muscles partially contracted all the time—this saves us time and conscious attention in carrying out repetitive actions. (Really, our nervous system is trying to be helpful!)
This learning process—that of developing what we refer to as muscle memory—allows us to go through the activities in our daily lives easily and efficiently. Unfortunately, if we tend to repeat unnatural, potentially damaging postures or movements—like certain types of athletic training, heavy lifting, or repetitive daily activities like sitting at a desk or carrying our baby on one side—our nervous system will learn those too. Our automatic neuromuscular learning process doesn’t discern what is good or bad for us—it just notices what we tend to repeat, and makes it automatic.
As our nervous system gradually learns to keep our muscles tight, gamma loop activity adapts. This feedback loop in our nervous system regulates the level of tension in our muscles. As our brain keeps sending the message to contract our muscles, gamma loop activity adapts and increases the resting level of tension in our muscles. Meanwhile, our proprioception (how we sense our body) adapts so that we’re not aware of the increased level of tension in our muscles.
This innate process of muscular learning takes place throughout our lives. It typically happens so gradually that we’re not aware of it until we notice the effects: tightness, pain, unnatural posture, limited movement, or structural damage to our joints and connective tissues.
How to use Clinical Somatics exercises to alleviate sciatica and piriformis syndrome
To prevent and alleviate sciatica and piriformis syndrome, you need to release the chronic muscle contraction in your lower back and gluteal muscles, and retrain damaging posture and movement patterns that could be causing compression of your lumbar spine.
If you try stretching or getting a massage to release your tight muscles, you’ll likely find that these approaches provide only temporary lengthening of muscles. Your muscles will tighten back up within a few hours due to the stretch reflex. Static stretching and massage do not change the messages that your nervous system is sending to your muscles to stay tight—active movement is necessary to retrain the nervous system.
The most effective way to reduce the tension in your muscles is with a movement technique called pandiculation. The technique of pandiculation was developed by Thomas Hanna, and is based on how our nervous system naturally reduces muscular tension. Pandiculation is the reason why Hanna’s method of Clinical Somatic Education is so effective in releasing tension and relieving pain. Hanna created many self-pandiculation exercises that can be practiced on your own at home.
Pandiculation sends accurate feedback to your nervous system about the level of tension in your muscles, allowing you to change your learned muscular patterns, release chronic muscle tension, and retrain your proprioception. You can read more about pandiculation in this post.
If you’ve learned Clinical Somatics exercises from my online courses or from another Certified Clinical Somatic Educator or Hanna Somatic Educator, you can use this section to help guide you in releasing the muscles that are causing your sciatica or piriformis syndrome. If you’re new to Clinical Somatics, the best place to start is the Level One Course.
Here are the exercises from the Level One Course that most directly relieve sciatica:
Arch & Flatten: I recommend practicing this every day. It’s best to begin your practice with this exercise, because it gently releases the lower back muscles and prepares you for the rest of your practice.
Back Lift: If you have sciatica or piriformis symptoms on both sides, then practice this on both sides. If you have symptoms only on one side, try doing this exercise (and the following exercises) only on that side to release the tight muscles and balance out your tension and posture. To do this, turn your head away from the side on which you experience symptoms. So, when doing the full movement, you’ll be lifting up the leg in which you feel symptoms. Only lift up your leg as high as is comfortable, and if it’s not comfortable, skip it for now. Be sure to lower your leg down as slowly as you possibly can.
Side Curl: This exercise releases the obliques; however, these can play a role in sciatica if your obliques are tighter on one side, causing you to hike one hip up or bend to that side. So if you have symptoms on one side, practice the Side Curl on that side. To do this, lie down on your non-painful side, and practice this exercise curling up to the side on which you have symptoms. Really try to get a sense of the muscles on the side of your waist contracting, then release them as slowly as you possibly can—resist gravity as you lower down. Completely relax for a few moments before repeating the movement.
One-Sided Arch & Curl: This exercise gives you the opportunity to do the Arch & Curl while focusing on just one side at a time. If you have symptoms on both sides, then practice this exercise on both sides. If you have symptoms on one side, lift up your knee on that side, and practice the exercise.
Iliopsoas Release: Tightness in the iliopsoas is very common, and it can compress the lumbar spine. If you have symptoms on both sides, then practice this on both sides. If you have symptoms on one side, practice this exercise by lifting up the leg in which you have symptoms.
Hip Rotation: The External Hip Rotator Release will help you to gently release your gluteal muscles. Practice this on both sides if you have symptoms on both sides. If you have symptoms on one side, practice this on the side in which you have symptoms.
And a few more exercises from the Level Two Course:
Lower Back Release: This is a wonderful exercise that gently releases the lower back, gluteals, and hamstrings. The more slowly you do this exercise, the more benefit you’ll get.
Proprioceptive Exercise 1: This exercise helps you to retrain your sitting posture, which is important for sciatica sufferers. Practice this to become aware of your sitting posture and of tightness in your lower back that could be causing your symptoms.
Gluteal Release: This is an important exercise for both sciatica and piriformis syndrome sufferers. Practice it on both sides if you have symptoms on both sides, or if you have symptoms on one side, practice it just with that side.
Standing Hamstring Release and Seated Hamstring Release: When you’re comfortable with the Lower Back Release and the Hamstring Release, you can practice these exercises to release your lower back and hamstrings further. If these exercises are not comfortable for you, then skip them for now.
Finally, be aware of how you’re using your body as you go through your daily life. Your progress with the exercises will be slower if you continue to do activities or habitual postures that are keeping you stuck in your patterns of tension and exacerbating your symptoms. Notice the tension that you hold in your lower back, as well as how you might be using the sides of your body differently when you:
- Stand for a few minutes: Do you hold tension in your lower back? Do you lean to one side?
- Carry your bag or your child: Do you hold tension in your lower back? Do you always use the same side?
- Sit at a desk: Do you hold tension in your lower back? Do you lean to one side, or cross one leg over the other?
- Relax on your couch: Do you lean to one side or lie on one side?
- Sleep: Do you sleep more on one side than the other, or do you sleep on your stomach? Sleeping on your back is best; put a pillow under your knees if that makes you more comfortable.
Ready to start learning?
If you’d like to learn Clinical Somatics exercises at home, the best place to start is the Level One Course. This online course teaches the exercises through video demonstrations, audio classes, and written explanations.
Recommended reading:
The Pain Relief Secret: How to Retrain Your Nervous System, Heal Your Body, and Overcome Chronic Pain by Sarah Warren, CSE
Somatics: Reawakening the Mind’s Control of Movement, Flexibility and Health by Thomas Hanna