How to Prevent and Alleviate Spinal Degeneration
Spinal degeneration refers to any breakdown or structural change in our spinal discs and vertebrae. The degeneration is virtually always the result of our chronic muscle tension, posture, and how we move and use our body on a regular basis.
Spinal degeneration can occur at any age, but the rate increases with age simply because the longer we misuse our body, the more likely it is to gradually break down.
The good news is that spinal degeneration is not inevitable; it’s just one of the negative effects of poor posture, imbalanced movement patterns, chronically tight muscles, and repetitive strain.
Have you been to the doctor and gotten a confusing or scary diagnosis that uses the words herniated, facet joint, osteophyte, radiculopathy, or stenosis? In this post we’ll clarify what all those terms mean so that you can understand what’s going on in your spine. We’ll also talk about why this degeneration occurs, and how you can alleviate your symptoms and prevent future damage to your spine with neuromuscular education.
Why do our spines break down?
Spinal problems are among the most common issues resulting from dysfunctional posture and movement patterns. Made up of 24 articulating vertebrae, plus the fused sacral vertebrae and bones of the coccyx, the spine is a miraculous feat of engineering. It allows us to bend forward and backward, side to side, and twist from right to left. The vertebral column protects the spinal cord while bearing a great deal of weight and absorbing shock as we run, jump, and lift heavy objects.
If we maintain healthy, balanced posture and movement throughout our lives, we should suffer little to no spinal degeneration. The problem is that because of muscle memory—the automatic way that our nervous system learns and remembers muscular patterns—we tend to build up chronic muscle tension and gradually adopt dysfunctional posture and movement habits over time. It takes a great deal of conscious attention, awareness, and movement training to avoid developing these issues.
For example, let’s say you have a job that requires heavy lifting. Not only do you put repetitive strain on your lumbar spine every day, but over time the muscles in your lower back become increasingly tight. The tight muscles compress your spine, bringing your vertebrae closer together and putting pressure on your intervertebral discs and facet joints.
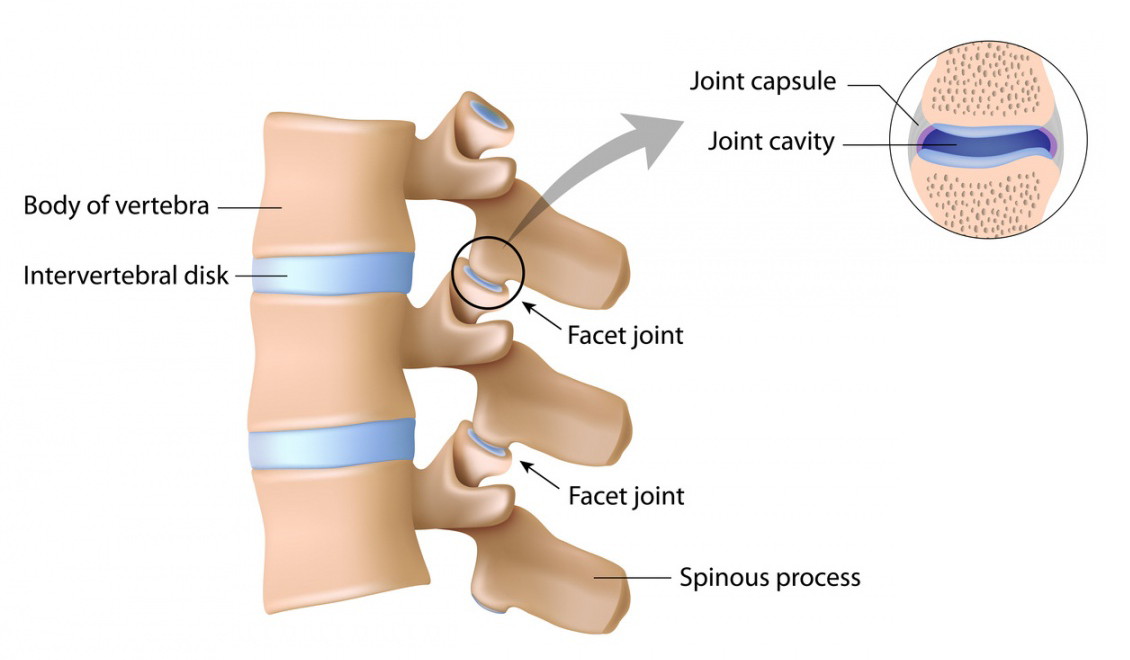
This compression causes the discs to slowly break down and become displaced, and the cartilage in the facet joints to wear away. Once this protection is gone, bone spurs develop on the vertebrae in order to stabilize the joints. Bone spurs, herniated discs, and thickened ligaments can cause stenosis, a narrowing of the spaces through which the spinal cord and spinal nerves pass. When the spinal cord or spinal nerves are impinged, you may experience pain, numbness, weakness, and balance or walking issues.
Our bodies do not break down for no reason. All of these degenerative structural changes occur simply because of the way we habitually use our bodies, so most of the time they are entirely preventable.
Disc degeneration
The discs that sit in between each vertebra are incredibly strong and resilient. Each is made of a tough outer layer of collagen fibers, called the annulus fibrosus, surrounding a soft core of a gel-like substance called the nucleus pulposus. The two structures work together to distribute pressure across the disc; this provides essential cushioning between the vertebrae and allows for bending, twisting, shock absorption, and weight bearing.
Thinned disc: The more the discs are compressed, the looser and weaker the fibers of the annulus fibrosus become, and tears can develop in the annulus. In addition, the nucleus pulposus can lose fluid. Both of these conditions contribute to discs thinning over time.
While this may sound like permanent damage, degenerative discs can heal if given the chance. The inflammatory process automatically kicks in to repair the disc, and if compression on the spine is reduced and muscular patterns are improved, degenerative discs can heal and resume their normal size and function. However, the annulus fibrosus has a limited blood supply, so doctors estimate that the healing process can take up to two years.
Bulging disc: When compression is constant, a disc may bulge or protrude from its normal boundaries. Sometimes it will press on a nerve root or the spinal cord, causing pain or another nerve sensation. If the bulge doesn’t press on nerve tissue, you may not feel anything at all.
Herniated disc: This is the same as a ruptured disc. If a disc is put under a great deal of strain from constant compression or a sudden increase in pressure, the contents of the nucleus pulposus can push out through a tear in the annulus. If the herniation presses on a nerve root, you may experience pain, numbness, or weakness.
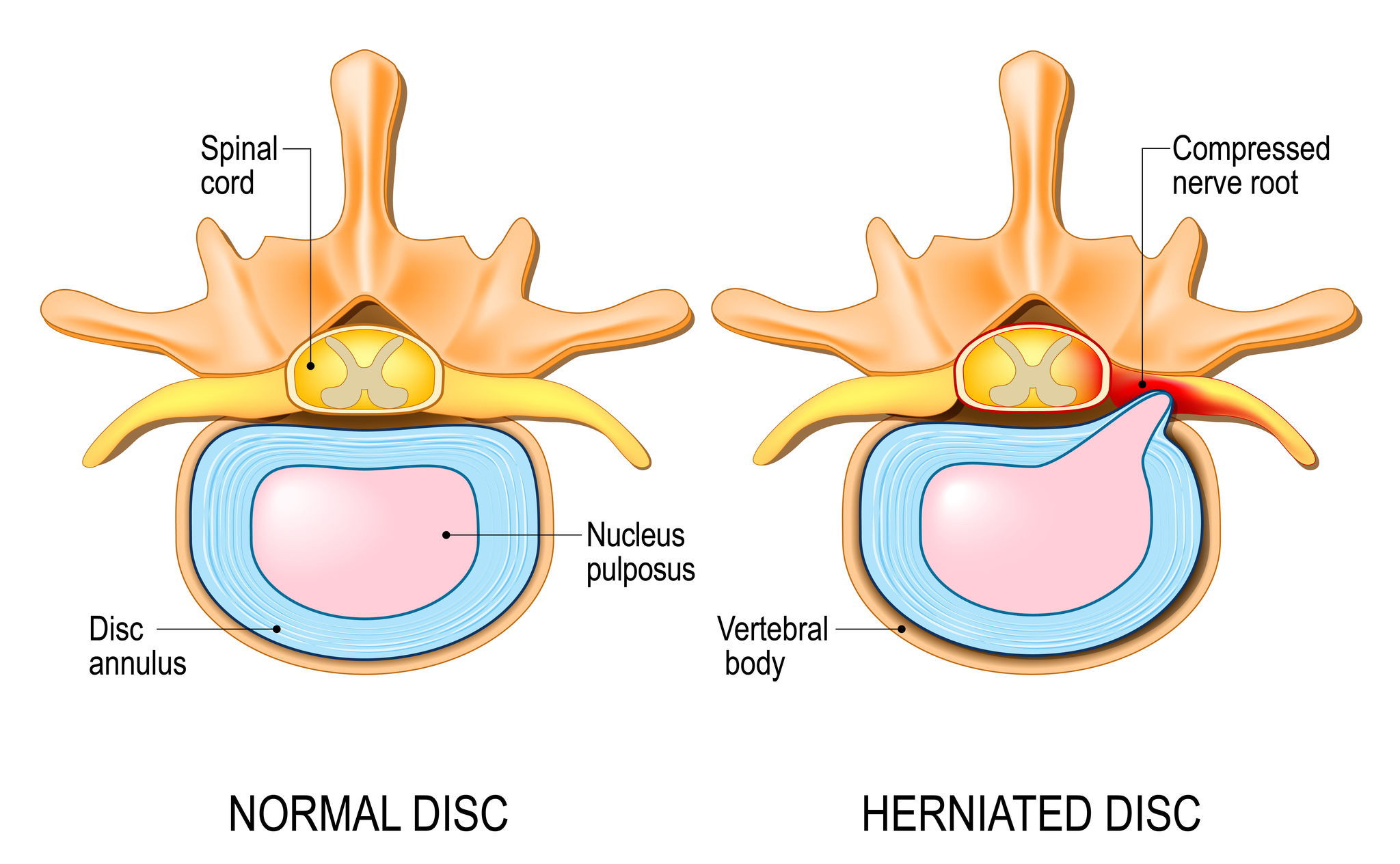
Facet joint syndrome
The facet joints in between each vertebrae (see first diagram in this article) allow the spine to bend and twist. With constant compression or imbalanced posture and movement, the cartilage in the facet joints can wear away. When this protective cartilage is gone, the joints can become inflamed, stiff, and painful, and movement of the spine is difficult.
Swelling and enlargement of these joints is called facet hypertrophy. In addition to pain and stiffness in the joint, the swelling may press on nerve roots, causing radiating pain and other nerve sensation.
Osteophytes
When intervertebral discs degenerate and facet joint cartilage is worn away, the vertebrae come into direct contact with each other. When bone rubs against bone, the body attempts to heal itself by growing osteophytes (bone spurs) in order to protect and stabilize the joint. While you may feel no symptoms, osteophytes can sometimes lead to pain, stiffness, and nerve sensation.
Spinal stenosis
Stenosis is an abnormal narrowing of a passage in the body. In the spine, central stenosis is a narrowing of the main central canal through which the spinal cord travels. Foraminal stenosis is a narrowing of the passageways through which the spinal nerves exit the spinal cord and travel to the extremities.
Spinal stenosis is most often caused by structural changes due to wear-and-tear: herniated discs, facet hypertrophy, osteophytes, and thickened ligaments all contribute to a narrowing of spinal pathways. Symptoms of spinal stenosis include numbness, tingling, weakness, localized or radiating pain, headaches, dizziness, loss of balance, limited mobility, muscle cramping, stiffness, and loss of bowel or bladder control.
Spondylolisthesis
Spondylolisthesis is the displacement of one vertebra compared to another. Anterolisthesis is forward displacement, retrolisthesis is backward displacement, and lateral listhesis or laterolisthesis is lateral (sideways) displacement. Symptoms of spondylolisthesis include pain and muscle tension in the lower back, buttocks, and legs; nerve sensation in the legs; muscle spasms; compensatory kyphotic (leaning forward) posture; and changes in gait.
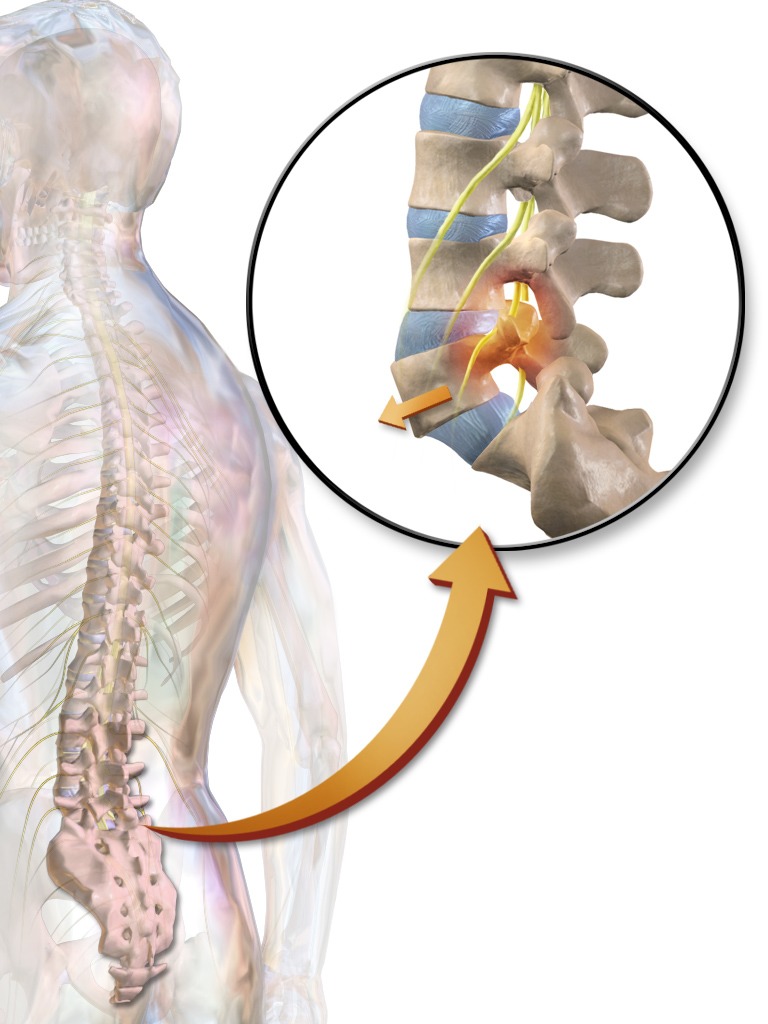
Radiculopathy
Radiculopathy occurs when a spinal nerve is compressed at or near the root of the nerve as it exits the spinal cord. We’ve been talking about radiculopathy throughout the previous definitions; it’s a common symptom of herniated discs, facet hypertrophy, osteophytes, spinal stenosis, and spondylolisthesis.
Sciatica is the most common type of radiculopathy. When the sciatic nerve is compressed, you may feel nerve sensations like tingling, numbness, pain, burning, weakness, or loss of muscular control in your buttocks, legs, and feet.
If you’re experiencing these nerve sensations elsewhere in your body, you can get a good idea of where your nerve compression is occurring by looking at the dermatome map below. A dermatome is an area of skin innervated by a single spinal nerve. To use the map, identify where you feel nerve sensation on your body, and find it on the diagram. The corresponding spinal nerve, labeled in the diagram, is the likely source of nerve compression.
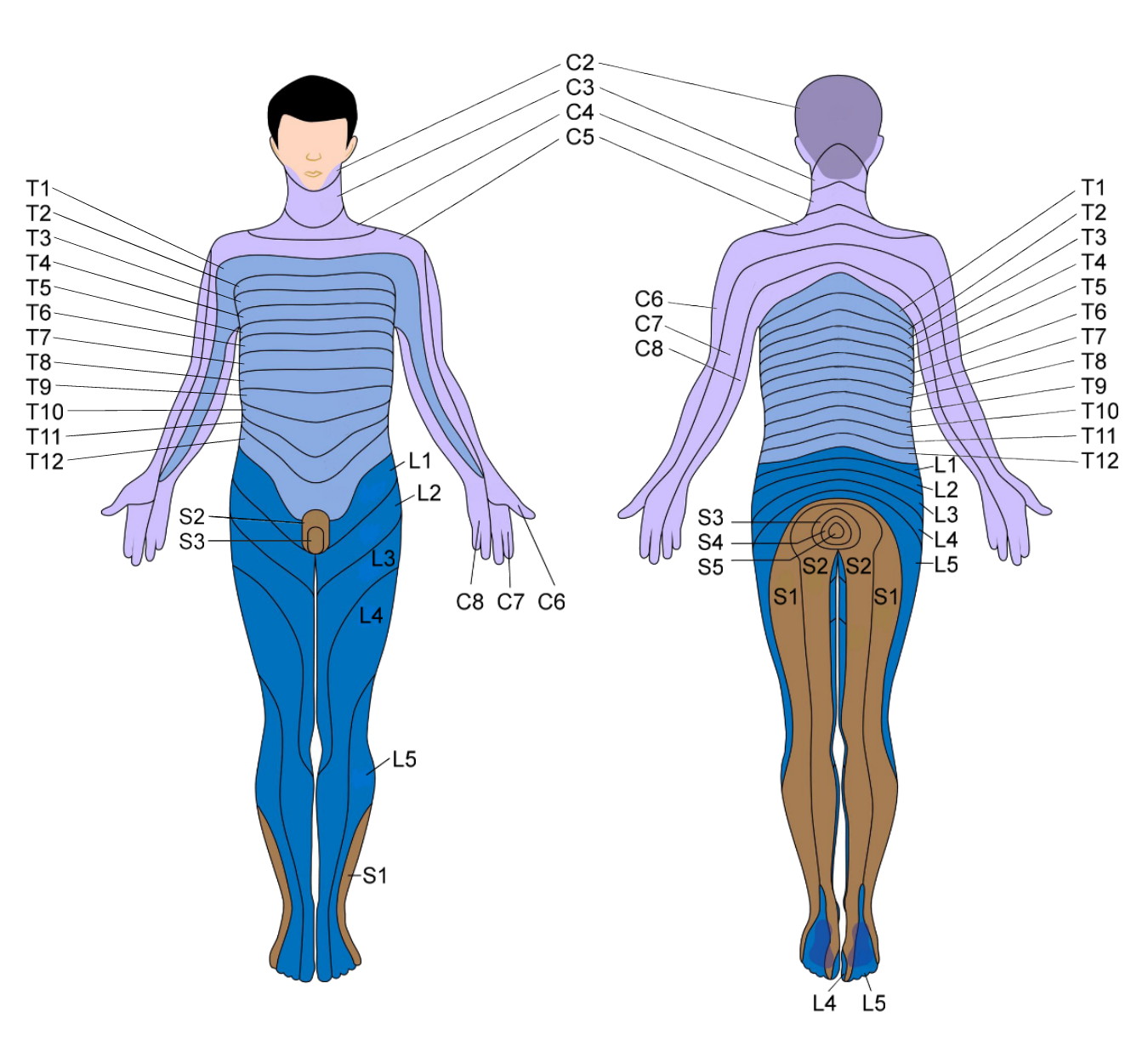
How to prevent and alleviate spinal degeneration with Clinical Somatics
The keys to preventing and alleviating degeneration of your spine are to:
- Release the chronic muscle tension in your back and neck that is compressing your vertebrae and discs
- Correct imbalances in your posture and movement that put unnatural strain and pressure on your spine
- Use proper body mechanics when lifting heavy objects
Strengthening your core muscles may add to your chronic muscle tension; do strength-building exercises with care and read this post about core strength. Static stretching may temporarily lengthen your muscles, but they’ll start tightening up within a few hours as your stretch reflex regains normal function. Chiropractic adjustments can realign your vertebrae temporarily, but your habitual muscular patterns will pull your spine out of alignment again within a few hours or days.
If you read this blog often or are familiar with Clinical Somatics, you know that the most effective way to release chronic muscle tension and improve your posture and movement is with pandiculation. Pandiculation works with your nervous system to reduce the resting level of tension in your muscles and retrain learned posture and movement patterns.
If you want to learn pandiculation exercises that reduce chronic muscle tension in the back and neck, improve posture, and prevent and alleviate spinal degeneration, the online Level One & Two Courses are the best way to start.
Here are the exercises in Level One & Two that most directly address spinal compression and alignment:
Level One:
Arch & Flatten
Back Lift
Arch & Curl
Side Curl
One-sided Arch & Curl
Iliopsoas Release
Diagonal Arch & Curl
Washcloth
Flowering Arch & Curl
Level Two:
Head Lifts
Lower Back Release
Proprioceptive Exercises 1, 2, 3, & 4
Diagonal Curl
Seated Twist
Standing Hamstring Release
Seated Hamstring Release
Head & Knee Lifts
Remember, spinal degeneration is not an inevitable part of the aging process! The more you are able to keep your core muscles released and your posture and movement balanced, the less likely you will be to suffer the painful effects of spinal degeneration.

