Sciatica and Piriformis Syndrome:
A Functional Perspective
What are Sciatica and Piriformis Syndrome?
Sciatica and piriformis syndrome describe pain and other symptoms resulting from irritation of the sciatic nerve. Symptoms can be experienced in the lower back and down either or both legs, even to the toes. Symptoms may include pain, shooting pains, burning, tingling, cramps, weakness, numbness, and loss of muscular control. Approximately 40% of the population may experience sciatica symptoms or piriformis syndrome in their lifetime.1
The sciatic nerve is the largest and thickest nerve in the human body, and it is responsible for much of the sensation and motor control of the legs and feet. Nerves exiting the spine between the fourth lumbar vertebra and the third sacral vertebra come together to form the sciatic nerve, which runs through the buttocks and all the way down each leg.
Sciatica (formally referred to as lumbar radiculopathy) occurs when the sciatica nerve is compressed as it exits the spine.
Chronic tightness or spasm in the piriformis muscle can also compress the sciatic nerve, causing piriformis syndrome. Many of the symptoms of sciatica and piriformis syndrome are the same; the distinction is made based on where the nerve compression occurs.
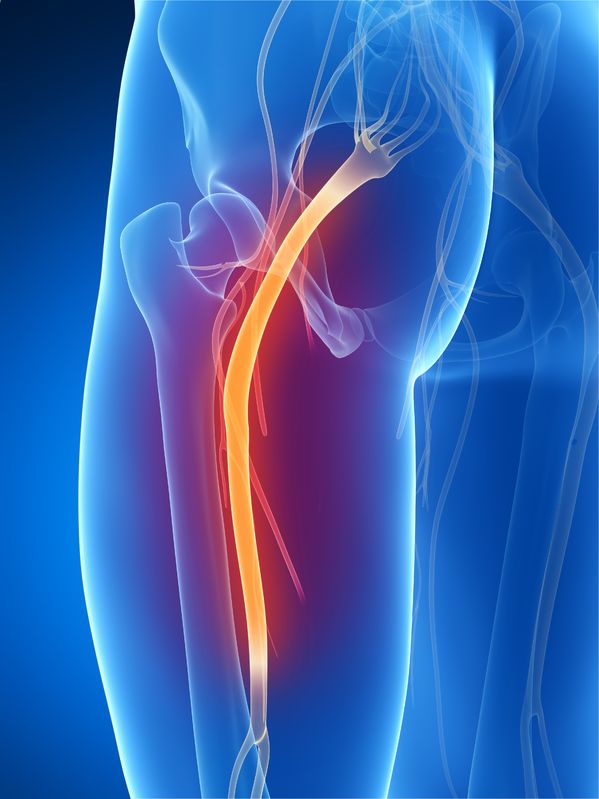
The sciatic nerve
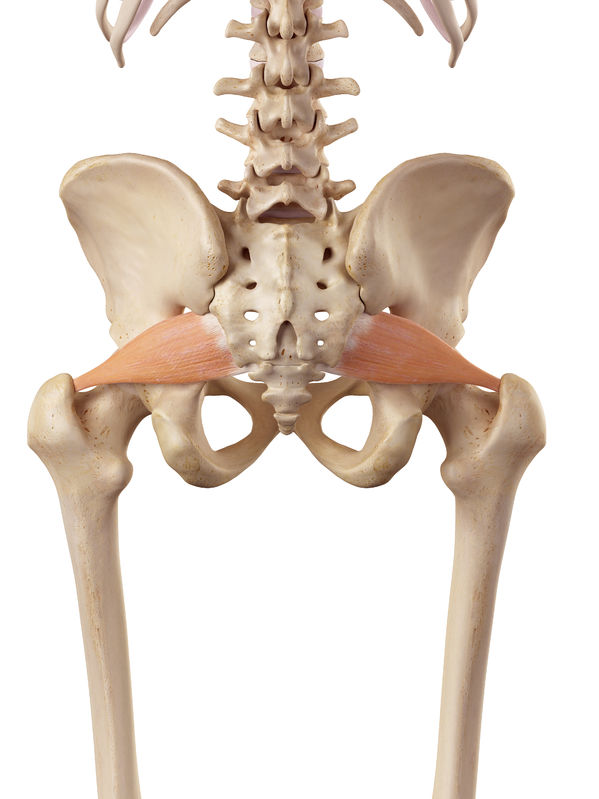
The piriformis muscle
Causes of Sciatica and Piriformis Syndrome
In about 90% of cases, sciatica is caused by a herniated disc compressing the root of the sciatic nerve.2 Other causes include degenerative disc disease, spinal stenosis, spondylolisthesis, pregnancy, tumors, or infection.
Sciatica typically begins as a functional issue. The structural issues that occur in the lumbar spine to cause sciatica are most often a result of the way we function: the way we habitually sit, stand, and move. Repetitive daily activities, athletic training, and heavy lifting can cause repetitive compression of the lumbar spine or make lower back muscles chronically tight, constantly compressing the lumbar spine. This compression can cause discs to thin and herniate, vertebrae to move out of alignment, the spinal canal to narrow, and bone spurs to develop.
Likewise, piriformis syndrome typically results from the way we use our bodies. Athletic training or imbalanced posture and movement patterns can cause the piriformis muscle (a gluteal muscle) to become chronically tight, compressing the sciatica nerve.
How to Prevent and Alleviate Sciatica and Piriformis Syndrome
The best way to prevent and alleviate sciatica and piriformis syndrome is to release chronic muscular contraction in the lower back and gluteal muscles, and retrain damaging posture and movement patterns that could be causing compression of the lumbar spine.
Clinical Somatic Education uses a highly effective movement technique called pandiculation that works with the nervous system to release chronic, involuntary muscle contraction. Clinical Somatics exercises also retrain posture and movement patterns, preventing pain and structural damage and allowing you to use your body in a natural, efficient way.
Clinical Somatics exercises are highly effective in relieving sciatica and piriformis syndrome. The Level One & Two Courses teach exercises that release involuntary muscular contraction in the lower back and gluteal muscles, relieving pressure on the sciatic nerve. The exercises are slow, gentle, and suitable for all ages and physical abilities.
References
1. Valat, J.P.; Genevay, S.; Marty, M.; Rozenberg, S.; and Koes, B. (April 2010). “Sciatica.” Clinical rheumatology. 24(2): 241–52. http://www.bprclinrheum.com/article/S1521-6942(09)00141-7/fulltext
2. Koes, B.W.; van Tulder, M.W.; and Peul, W.C. (June 2007). Diagnosis and treatment of sciatica. British Medical Journal, 334(7607): 1313–1317. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1895638/
